 
For this reason, in all patients with VPCs, one must perform a detailed clinical history of 12-lead EKG and chest X-ray. In some cases, VPC is the first manifestation of underlying structural heart disease. In asymptomatic individuals, VPCs may be initially identified on a routine physical exam by an irregular rhythm consisting of a premature beat followed by a compensatory pause with subsequent return of regular rhythm, or cardiac auscultation revealing a sharp first heart sound or splitting of S2 or on a routine office electrocardiogram. 
VPCs rarely may cause hemodynamic compromise leading to presyncope or syncope, mainly if they occur in sustained or frequent runs. Patients may often report a sense of abnormal neck pulsation with palpitations when they experience VPCs. In patients with pre-existing heart disease, frequent VPCs can cause dyspnea, angina, and palpitations. However, some patients will report fatigue, palpitations, lightheadedness, or dizziness. Most often, ventricular premature complexes are asymptomatic. Several factors are involved in this diversity, including coronary heart disease, African-American ethnicity, male gender, older age, hypertension, faster sinus rates, lower serum potassium or magnesium levels, and lower education level. The variability in the reported data differs due to the different monitoring techniques and duration used to calculate VPCs prevalence. Those patients with coronary artery disease, the prevalence was comparatively higher, with 58% in men and women 49%. According to the Framingham Heart Study, the prevalence of VPCs was found to be higher in one hour continuous EKG monitoring with 33% being the men and 32% women with no history of any coronary artery disease. 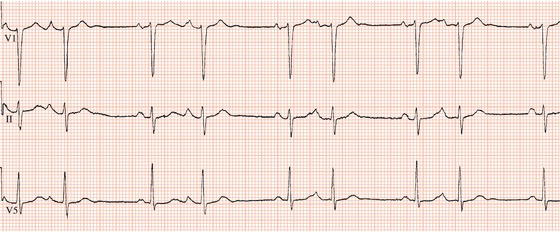
Researchers conducted a study in a healthy military population with a recording of 12-lead EKG that showed almost 0.8% of subjects with ventricular premature complexes with a 0.5% prevalence in the population under the age of 20 years and in those over the age of 50 years it was found to be 2.2%. Those VPCs that originates in the left ventricle are usually associated with a right bundle branch block (RBBB), and VPCs that arise in the right ventricle show a left bundle branch block (LBBB) pattern. The 12-lead EKG helps to identify the precise location of the origin of VPCs only by the morphology of ectopic beats. Premature ventricular contractions classify according to coupling interval (early and delayed), QRS duration (wide and narrow), morphology, and complexity. However, in certain instances, a QRS complex of duration less than 120 ms can occur, leading to activation of both ventricles "synchronously" because of electrical stimulus from one of the fascicles through a specific conduction system. The VPCs usually originate from the ventricle that leads to a prolonged QRS complex duration greater than 120 ms because of the delay in the spread of activation to the contralateral ventricle through non-specialized myocardium. The morphology of VPCs is highly variable, and it depends upon its place of origin, underlying structural disease, or the use of antiarrhythmic drugs. Reports show that frequent VPCs can cause progressive left ventricular (LV) dysfunction and dilation, which may return to normal after successful catheter ablation of the VPCs. They can present in patients both with and without preexisting cardiac disease. They are common and can occur in a wide variety of clinical scenarios and a diverse population. Ventricular premature complexes (VPCs), or premature ventricular complexes/contractions (PVCs), are ectopic beats that arise from within the ventricles. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
